I arrived in Santa Cruz de la Sierra, Bolivia’s second largest city, confident in my mission. I was a member of the Northwestern Trauma and Surgical Initiative (NTSI), a group dedicated to surgical access. I was to work on an established project with Santa Cruz’s government, hospitals, and physicians to help build a foundation for a trauma system to improve patient care and outcomes. Another NTSI team member laid the groundwork for my visit; she had spent the past year gathering quantitative data about the trauma burden in and around the city of Santa Cruz. My job was to complement this data with patient experiences. I would spend two months interviewing trauma patients in the hours after their injury to ascertain their interactions with the emergency medical system as well as their values and beliefs on trauma.
I arrived with knowledge that I thought would prepare me for my experiences in Bolivia. I knew that 70% of the world’s population has no access to surgical care. Furthermore, I understood that low- and middle-income countries (LMICs) are unfairly burdened by trauma; for every one injury-related death in high-income countries, there are nine in LMICs (1). However, I soon came to realize that no quantity of statistics nor World Health Organization reports could prepare me for the despair and suffering found in those who could not heal for lack of ‘dinero’ (money). In hospitals filled with providers who took an oath to do no harm, patients’ fates were determined by pieces of paper to which we have given such significant value that care could not be initiated without them.
 Imagine the emergency room (ER). A patient arrives and is evaluated by a physician. The family is given a prescription. They run off to collect supplies at the pharmacy, and care does not commence until the family returns with a bag filled with bandages, IVs, needles, medications, and orthopedic and surgical devices. This ‘bolsa’ (bag), hangs from the edge of the patient’s bed, defining the quantity and quality of care he or she will receive. If the bag is large, the patient is in luck; if it is small, his or her care will undoubtedly suffer. In Bolivia, money determines who lives and who dies, who becomes whole and who lives permanently scarred. Money determines all…
Imagine the emergency room (ER). A patient arrives and is evaluated by a physician. The family is given a prescription. They run off to collect supplies at the pharmacy, and care does not commence until the family returns with a bag filled with bandages, IVs, needles, medications, and orthopedic and surgical devices. This ‘bolsa’ (bag), hangs from the edge of the patient’s bed, defining the quantity and quality of care he or she will receive. If the bag is large, the patient is in luck; if it is small, his or her care will undoubtedly suffer. In Bolivia, money determines who lives and who dies, who becomes whole and who lives permanently scarred. Money determines all…
The Artist was born and raised in Santa Cruz de la Sierra, but spent most of his adulthood in Barcelona, painting. He said he was happy. A few years ago, his mother asked him to come home; she was sick and alone. He did, and things were okay.
I met The Artist as he lay in bed, his legs held together by external fixation devices wrapped in bloody bandages. His left arm was casted up to his shoulder. I could not help but notice his sheets, childish and colorful. I looked around, feeling embarrassed upon realizing each bed had a different set. Uniformity is a privilege of hospitals that have money to buy in bulk. Despite the long month he had spent bedridden after his injury, The Artist was sharp and his eyes gleamed with an unshakeable intelligence. I asked him what he thought of the Bolivian health care system.
“Si no tienes dinero, te mueres, (If you don’t have money, you die).”
I asked him what he meant, but he only elaborated with a shrug of his shoulders.
“When do you go home?”
He tapped on his right knee. “Cuando yo tenga la plata. (When I have the money)” Both his kneecaps had shattered in the collision, and he only could afford to repair one of the two. For now, his right leg lay motionless on the bed, unable to extend.
“How much?” I asked.
“Cien dolares (100 dollars).” He responded.
I asked him where he would find the money.
He doesn’t know, he says. He is already in so much debt.
The Dreamer and The Artist became friends as they lay immobilized next to one another. The Dreamer is a 19-year-old boy with bright brown eyes and a friendly disposition. His vitality, laugh, and smile starkly contrast against his swollen leg held in traction by an unsightly wooden device comprised of blocks, bandages, and water-filled coke bottles. He dreams of becoming a doctor despite never completing high school. In his misfortune, he was born in the countryside, where it was impossibly expensive to send a child to a university in the city. The Dreamer could not get better. He could not go home. He did not have the money to do so.
A week prior, he had been riding on his friend’s motorcycle when they were forced to swerve away from an oncoming car. The Dreamer broke his femur. Upon arrival to the hospital, his mother found the money for the initial operation. The surgeons inserted a nail into his distal femur to allow them to put his leg in traction and reposition the broken bone. However, traction was intended as a temporary fix until the surgeons could perform a second operation to insert rods to hold his femur together. As of the moment I spoke with him, there were not yet plans for the permanent fix. I asked him why not…
“Es mucha plata, (It’s a lot of money)”, he said dejectedly.
“What are you going to do?” I asked.
He responded by saying that his mom is trying, but she has no idea where she will find the money. I sensed that they are very far from a solution. Until then, he will lay in bed, a nail driven through his leg, and two coke bottles holding his femur in place. What once was a temporary fix had turned into a prison, because here in Bolivia, you buy your medical supplies and operations prior to receiving care. If you can’t—you wait.
Within these exceptionally difficult conditions, I witnessed truly altruistic medical care. I saw physicians dip into their pockets to cover medications, treatments, and sizeable operations. However, an unbalanced scale exists in Bolivia. The needs far outweigh the resources, and with every good deed, 10 patients you cannot help appear. This crushing burden can take a toll on healthcare providers, as I witnessed during a shift in the ER of Santa Cruz de la Sierra’s busiest hospital.
I had been invited to spend an afternoon in the ER with a third-year internal medicine resident. Inside, I found confusion, heat, and a scent of fear, sweat, and antiseptic, which contrasted sharply with the lazy drizzle and cool weather outside. The resident explained the set-up of the department: one large room, with 24 beds packed together on the right (the general ER) and five more stretchers on the left containing the sickest patients, usually intubated, precariously balancing on the precipice between life and death. One of two hallways through which one could enter was packed with eight more patients and their families. He pointed to the hallway. “That,” he said, “is where we keep the TB patients.” I watched as patients and families walked through this narrow, congested hallway. “Try to find a mask if you go in there,” he instructed me. I nodded.
The department was chaotic. Patients moaned in pain, left unattended. There was a man with third degree burns to his face, who said he had waited in the ER, left in limbo in the unsanitary environment, for two days. I watched an intern manually bag an intubated patient for hours. There were five individuals in need of ventilation but only four ventilators. The patient was transferred during my shift. Not because of the lack of a ventilator, but because he had a suspected stroke, and the CT scanner at this hospital had been broken for two days. Keep in mind, this is one of only two general tertiary care facilities intended to provide care for a population of 2.5 million, and there was no functioning CT scanner.
After six hours, I felt dead and depressed. When I think back on my experience, one moment overwhelmingly comes to mind—
The resident looks up at me. He shrugs his shoulders and waves his hands at the team who disperse back to their own jobs. His lips turn up and he gives me a conciliatory smile, as if to say, it’s okay, we did our best. He steps away, and I stare transfixed by the body. His skin is brown, and he is of a small build, lean and wiry, someone who spent his days working in the fields. He looks young; he can’t be more than 45, only flecks of gray in his hair. He is bare from the stomach up, and his pants are stained with urine and feces. An intubation tube hangs from his slack jaw, his eyes glazed and lifeless. I hear a wail from behind me. The wife and two daughters stare at their husband and father. They stare at the man they love, and my heart breaks for them. There lies their father, a symbol of strength and safety, filled with tubes, covered in excrement. This would be their last memory of him. I watch as the attending physician crosses over to them and says the words I will never forget, “Tienes que pagar por los tubos y medicaciones, no podemos reutilizarlos, (You have to pay for the tubes and medications, we can’t reuse them.)” They do not respond. They cry. They stare. I cannot fathom the pain they are feeling.
I often think back to The Dreamer’s response when I asked him how he would pay for his care. “Tienes que tener fe. Fe en Dios. (You have to have faith. Faith in God).” I personally am not religious; however, I understand his sentiment. If medicine won’t save you, you need to believe someone will.
——————————
Sometimes I think back to something my mentor said to me before I left for Bolivia. She bought me a journal, and as she handed it over, she said, “Find something that gives you fire, something that burns you, but doesn’t consume you.” At that moment, I nodded my head, but I did not comprehend the meaning of her words. This past summer, I found my fire. In my ignorance, I underestimated the strength of the flame, and I was burned. Six months have passed since I began this journal entry, and in that time, my anger and confusion have given way to understanding and hope. The experiences of patients, like those I interviewed, will be the foundation on which we build our trauma system. I will never look back on these stories without feeling pain, but perhaps that is what my mentor intended to convey. These patients and their stories give me fire, they burn me, and that is a gift I am blessed to have discovered.
Something that has never wavered since my arrival in Santa Cruz is the belief that the NTSI will play a critical role in establishing an effective and cost-efficient trauma system for the city of Santa Cruz. I believe this for three reasons:
- The strategy the NTSI has utilized in developing a novel trauma system.
- The plethora of talented and inspired Bolivian physicians, nurses, residents, students, and first responders.
- The potential cost effectiveness of trauma interventions.
From the very start, this project has been carried out with the utmost professionalism and cultural competence. All potential stakeholders are intimately involved in the project, including the local government, public and private hospitals, and an extensive network of inspired, talented, and dedicated healthcare providers. Furthermore, we are attacking a problem, preventable injury-related deaths, in a systematic and scientific manner. By 2018, members of the NTSI will have spent three years in Santa Cruz collecting quantitative and qualitative data, drafting legislation, and training first responders. In collaboration with stakeholders, we will utilize this accumulated information, as well as existing human capital, to design the best possible trauma system for Santa Cruz.
The interviews I collected this past summer will play a very small part in this process. Although the data is preliminary, certain themes became evident to me as an interviewer. For example, many patients did not trust public ambulances, instead choosing to use taxis no matter how severe their injuries. This suggests a potential high-yield intervention target, to provide education to taxi drivers on basic first responder skills and appropriate hospital triage based on injury severity. I also found many patients did not know the number to call for an ambulance. A unified call center is the logical next step, with widespread public awareness campaigns that provide education on the system’s function and purpose, to hopefully overcome the current level of mistrust. It is small themes like these that have arisen from my project that I hope will guide the trauma system development as we move forward.
Only now am I able to recognize that, in focusing on patient suffering, I failed to fully appreciate the skill, generosity, and empathy of many of the physicians I met while in Santa Cruz. The stakeholders at each of the hospitals were passionate and excited about the project. They had spent decades working in a resource-poor setting that had broken me in two months, yet their empathy did not waver. I think back to a surgeon who dipped into her pocket to buy supplies to suture the scalp of a little boy with a large laceration. Only days later she did the same to pay for clean dressings for a small boy of 15 years who had suffered third degree burns to much of his leg. Later that month, I met an orthopedic surgeon who worked tirelessly to find supplies for The Dreamer so he could finally receive his surgery after 20 days in traction. It is experiences with physicians like these that provide me with the faith that we have the right people in place to organize and implement a better trauma system.
We must also discuss our rate-limiting factor—money. In the US, the per capita Gross Domestic Product (GDP) is about 55,000 USD per person per year; in Bolivia, it is 2,900 USD (2). In the US, we spend about 9,500 USD on healthcare per person per year; in Bolivia, they spend 209 USD (3). Our economies are vastly different. It is unrealistic, therefore, to expect medical care to be the same.
However, our program development and implementation deals with systems. And systems do not have to be expensive. Our mission is to work with local healthcare providers, hospitals, and the government to create a trauma system that brings patients to the right place, at the right time, with the right care available. It does not have to be expensive—only efficient and effective. I truly believe that what our wonderful team is doing will save lives and decrease human suffering. I am incredibly thankful to have a small role in this process.
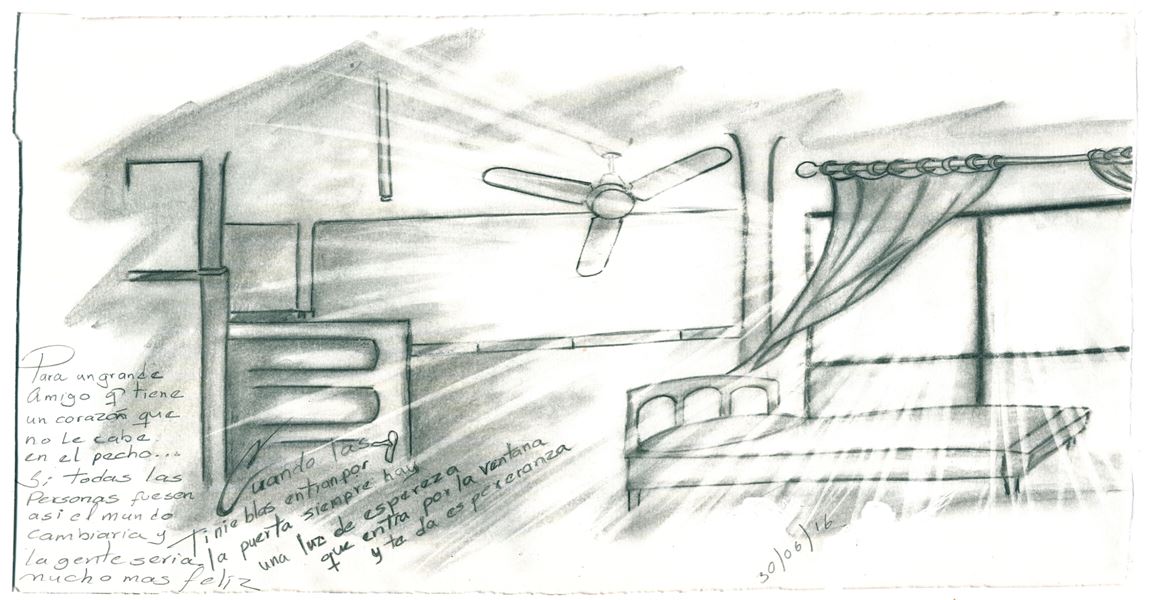
In my final days, The Artist gave me a drawing of the hospital room in which he had spent nearly a month bedridden. The inscription was as follows: “When the darkness enters through the door, always there is a light of hope that enters through the window and gives you hope.” We strive to be that hope. We strive to #bethechange.
References:
- Injuries and Violence, The Facts 2014. World Health Organization. Geneva Switzerland. 2015
- http://data.worldbank.org
- http://data.worldbank.org/indicator/SH.XPD.PCA
If you would like to learn more about the Bolivian Trauma Initiative or any of the Northwestern Trauma and Surgical Initiative’s many projects, please visit the following website: http://ntsinitiative.org.